News
San Diego Supercomputer Center Powers AI Model to Improve Prostate Cancer Care
Published February 27, 2026
By Kimberly Mann Bruch
Researchers and clinicians from six leading medical centers and academic institutions — including the University of California San Diego — have collaborated to develop a new artificial intelligence model of the male urinary tract that could make prostate cancer radiation therapy more precise and help reduce side effects, such as urinary complications.
The team used U.S. National Science Foundation (NSF) ACCESS allocations on the Expanse system at the UC San Diego School of Computing, Information and Data Sciences’ San Diego Supercomputer Center to construct a detailed MRI-based atlas of the urethra, the narrow tube that carries urine through the prostate. They tested this tool against a robust reference standard created by having four imaging and radiation experts reach consensus on the precise location of the urethra in scans from 71 patients.
“Our AI tool, developed with the help of NSF ACCESS allocations on SDSC's Expanse, automated contours of the urethra. This system substantially improves coverage of the true urethra compared to human physician contours. In our study, we showed that the AI tool typically identified 81% of the true urethra, while the physician version typically only covered 34%.”
— Dr. Tyler Seibert, UC San Diego Health radiation oncologist and associate professor
Lead author Yuze Song, an electrical engineering doctoral student in UC San Diego’s Jacobs School of Engineering, worked on the study alongside Tyler Seibert, MD, PhD, associate professor of radiation medicine and applied sciences at UC San Diego School of Medicine and radiation oncologist at UC San Diego Health, and an international team of collaborators.
“During radiation treatment for prostate cancer, it’s critical to avoid giving too much radiation to the urethra, as this can lead to serious urinary problems,” Seibert said. “On MRI scans, the urethra is tiny and often difficult to identify clearly — even for very experienced doctors. That uncertainty can lead to differences in how doctors plan radiation, potentially affecting treatment safety.”
By running their AI model on Expanse, the team automatically identified the urethra on MRI scans from all 71 patients. When tested on challenging cases, Seibert said that the AI-generated outlines could overlap the urethra anatomy, which may help reduce radiation toxicity during treatment.
“The AI system performed impressively — thanks to the power of Expanse,” Song said. “Trained on data from 11 MRI scanners across six hospitals, it produced urethra contours that were typically within about two millimeters of the expert standard — similar to or better than many human specialists. Even in the most difficult cases, the program still captured one-third of the urethra and deviated by less than three millimeters.” Song is a Ph.D. student in the Department of Electrical and Computer Engineering at the UC San Diego Jacobs School of Engineering.
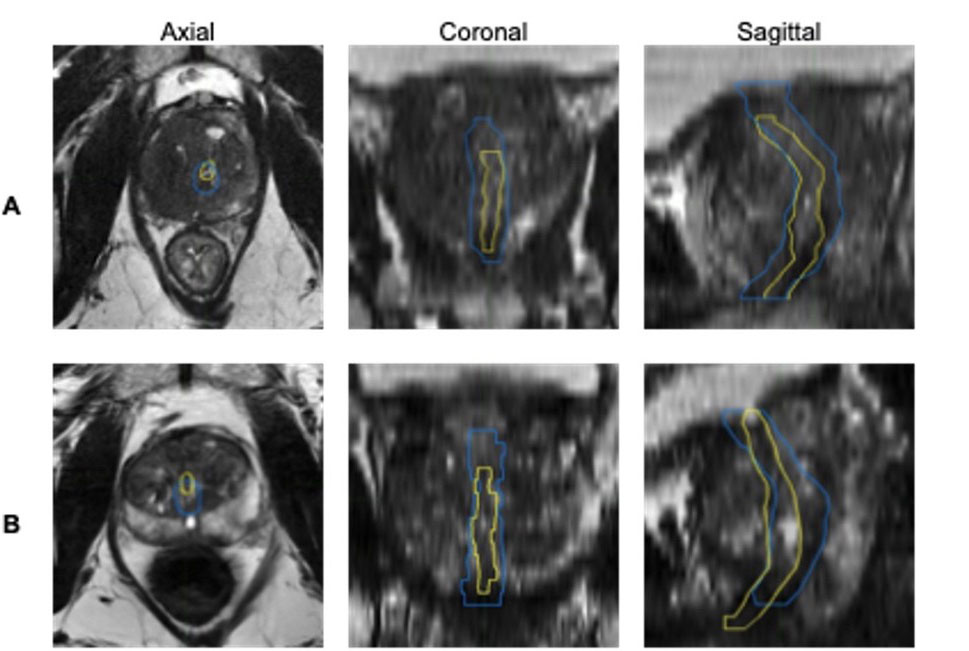
Side‑by‑side MRI images show how an AI system outlines the urethra compared with outlines drawn by a team of medical specialists. In each view (axial, coronal and sagittal), the yellow line shows the experts’ outline and the blue line shows the AI’s outline. Panel A shows one example where the AI only partly matches the expert outline, while panel B shows another example where the AI comes closer to the expert outline, especially along the edges. Credit: Yuze Song, electrical engineering Ph.D. student at UC San Diego
If validated in future clinical trials, this approach could make prostate radiation treatment more consistent across clinics and help minimize urinary side effects for patients.
Full study details appear in Radiotherapy and Oncology.
The time on Expanse was supported by NSF ACCESS (allocation no. MDE230005).

